More than 240,000 patient falls happen every year in UK hospitals
More than 240,000 falls are reported in acute hospitals and mental health trusts in England and Wales every year - that's 700 a day, according to the first nationwide audit of hospital inpatient falls.
The Royal College of Physicians’s National Audit of Inpatient Falls (NAIF), published at the British Geriatrics Society's autumn conference today, looked at acute hospitals in England and Wales.
The audit found there are more than 3,000 hip fractures being suffered by patients every year as a result of a fall in hospital.
The audit also found that the direct cost of hospital falls amounts to £15m a year, which equates to £92,000 for an 800-bed acute hospital trust.
Out of the 142 eligible hospital trusts and health boards that were invited to participate in the audit, 140 registered for the audit and 136 submitted valid data. The audit is based on data for 5,174 patients, submitted by 188 hospitals.
One patient’s experience of their fall in hospital still frightens them two years later. In the report, the patient stated: 'I was on the way to recovery, but I’d been in bed so long I was incredibly weak ... I went to wash my hands and I slipped. There’s an immediate shock of landing on your back.
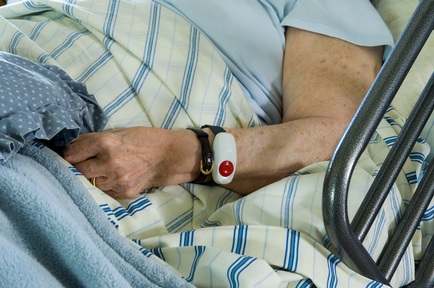
'Then the terrible thing was I realised I couldn’t move through lack of strength. I couldn’t reach the pull cords, and my voice was also very weak at the time, I couldn’t shout. I was on a cold tile floor and I started to get cold, and that’s when fear starts to strike you.
'It made me cautious in a very hesitant way. It was a major thing for me ... it hit me psychologically. It’s still there, still there, even 2 years on.'
Although all organisations have a falls prevention policy, the audit found that 32 per cent of these policies are being written in isolation and do not link to any other related policies, such as those on delirium, dementia and bone health. As a result the report recommends that all hospitals and trusts review their falls policy to take into consideration other policies dealing with areas such as dementia and delirium.
The report revealed that many hospitals failed to routinely assess for dementia (42 per cent) or to develop a care plan for those with cognitive impairment (67 per cent). Delirium was monitored even less routinely, with only 37 per cent of patients being assessed.
Dr Shelagh O’Riordan clinical lead, said: “This is the first time there has been a national audit of falls prevention in hospitals across England and Wales. Our results show that although there are pockets of really good care, many hospitals are not doing everything they can to prevent falls. I hope this inaugural audit is the first step to help reduce the number of falls currently happening in hospitals in England and Wales."
The report makes a number of recommendations to help hospitals reduce the number of patient falls. This includes:
• Ensuring those over the age of 65 years receive a lying and standing blood pressure check and take action if there is a substantial drop in blood pressure when a patient stands.
• Giving older patients a medication review, looking particularly for medications that are likely to increase their risk of falling.
• Assessing older people for visual impairment and have a continence care plan developed if there are continence issues.
• Getting all trusts and health boards to regularly audit whether a patient’s call bell is within reach of them.
• Ensuring that all patients who need walking aids have access to an appropriate walking aid from the time of admission.
Speaking on behalf of the British Geriatrics Society, Professor Adam Gordon said: “Many of the interventions described, such as ensuring availability of call buzzers, seem straightforward but can easily slip by the wayside in busy clinical settings. This audit will allow hospitals which are doing less well to reflect on their current practices and policies, and learn from those parts of the country which are doing better."
Latest News
 29-Jul-24
Dementia Bus gives carehome.co.uk staff insight into life with dementia
29-Jul-24
Dementia Bus gives carehome.co.uk staff insight into life with dementia
 27-Jul-23
UK's top home care agencies in 2023 revealed
27-Jul-23
UK's top home care agencies in 2023 revealed
 30-Nov-22
A quarter of older people keep their falls secret from family
30-Nov-22
A quarter of older people keep their falls secret from family
 29-Nov-22
'Covid-19 has not gone away' say terminally ill
29-Nov-22
'Covid-19 has not gone away' say terminally ill
 28-Nov-22
IT consultant who received poor care opens 'compassionate' home care business
28-Nov-22
IT consultant who received poor care opens 'compassionate' home care business